Allergic Conjunctivitis


What is Allergic Conjunctivitis?
What are the triggers of Eye allergy?
What are the types of Allergic Conjunctivitis?
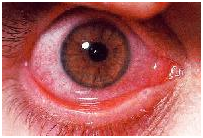


Seasonal Allergic Conjunctivitis & Perennial Conjunctivitis
Allergies to Animals
Vernal Kerato Conjunctivitis
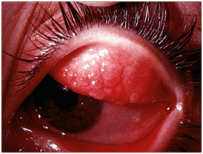


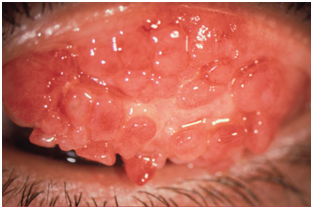


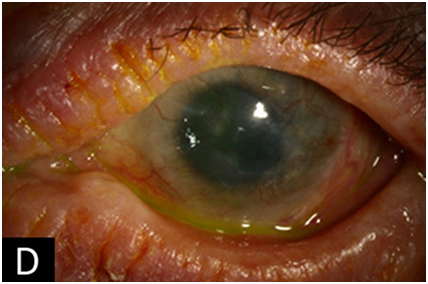
Giant Papillary Conjunctivitis
This is uncommon. It is an inflammation of the conjunctiva lining the upper eyelid.
It occurs in some people who have a small object on the eye – most commonly, a contact lens.
It affects about 1 in 100 wearers of contact lenses. The exact cause of the inflammation is unclear -it is possibly an allergic reaction to debris caught behind a lens or to poor lens hygiene.
It also sometimes develops after eye surgery.
Atopic Kerato Conjunctivitis


Contact Conjunctivitis
What are the Symptoms of Allergic Conjunctivitis?
1
Itching
2
Redness of eyes
3
Burning
4
Mild sensitivity to light (Photophobia)

5
Stringy or ropy discharge
6
Teary eyes with a watery discharge
7
Stinging

Are there any possible complications?
What is the treatment for Allergic Conjunctivitis?
Bathing the eyes
Bathing the eyes with an over-the-counter ‘eye bath’ may ease symptoms.
Try not to rub your eyes,
Try not to rub your eyes, as this can cause more inflammation.
Avoid the cause of the allergy
For example, if you have seasonal conjunctivitis then during the hay fever season try to avoid pollen by staying indoors as much as possible. Close windows, drive with windows shut and internal air circulation on in your car, and by wear wrap-around sunglasses when out.
If you use contact lenses
in general, do not wear lenses until symptoms have gone, and for 24 hours after the last dose of any eye drop or ointment. However, your doctor or optician (optometrist) will advise if you can wear lenses with certain types of drops.
Treatment for seasonal, perennial and animal-related conjunctivitis
Antihistamine eye drops
these are usually needed only twice a day. They have few side-effects and can be very effective in reducing symptoms.
Mast cell stabiliser eye drops
these have been around for a long time. They are also very effective and relatively free from side-effects. They need to be used frequently, as they are shorter-acting: four times a day or more.
Combination anti-allergy drops
These combination drops are not suitable for everyone. For instance, children under 12 and patients with raised pressure in the eye (glaucoma) should not use them. Your doctor or pharmacist can advise if they are safe for you.
Antihistamine tablets
These are taken to try to generally lower the allergic response in your body
Steroid eye drops
Steroid drops are very effective in eye irritation. They calm down irritation and inflammation quickly. However, they increase the risk of eye infection, which can rapidly become severe in the presence of steroid drops. They can also lead to glaucoma. Therefore they should only be used if other treatments fail, and they are normally only used under the supervision of an eye specialist.
Eye drops and contact lenses
most drops contain preservatives. However, in some cases preservative-free versions are available, as the preservatives may also cause eye irritation or allergy! Soft contact lenses should not be worn whilst the drops are being used, as the preservatives can be absorbed into the lenses and can further irritate the eyes.



